"To PE or not to PE, that is the question..."
Ruling out Pulmonary Embolism

Case
31 year old female presents to ED with sharp left sided chest pain and SOB which woke her from sleep.
2/52 history cellulitis and ulceration of right foot - received iv antibiotics last week but likely non-compliance with further oral antibiotics.
Worsening of infection, now unable to mobilise due to pain.
On examination: alert and orientated, Temp 38.2, BP 135/80, HR 110, RR 18, 97% RA
O2 sats directly after a brisk walk around the department: 97%
Chest clear, tender left sternal border - reproduced on palpation.
Ulcerated area on right foot with surrounding cellulitis. Right leg circumference 4cm greated than left leg, generally tender.
Normal chest xray, ECG and routine bloods except CRP 121
Differential for chest pain: PE vs costochondritis
Can pain on palpation rule out PE?
Presence of chest wall tenderness reduces the likelihood of PE but CANNOT be used to rule out the diagnosis (1)
Chest wall tenderness in the presence of a PE could be explained by:
- pulmonary infarct causes irritation and inflammation of the parietal pleura
- intercostal skin is also supplied cutaneous branches of the intercostal nerves that supply the parietal pleura
-
palpation of the chest wall could theoretically:
- a) apply pressure to the already inflamed and stretched parietal pleura
- b) and/or put pressure on a hyperalgesic area of skin supplied by the same intercostal nerve
Can lack of desaturation on exercise rule out PE?
There is no published evidence to support the use of measuring oxygen saturations after exercise in diagnosing PE (2)
Pulmonary embolisms cause a range of abnormalities in gas exchange:
- V/Q mismatch
- Reduced arterial PO2
- Increased alveolar-arterial O2 tension gradient
With increasing exercise intensity arterial PO2 decreases.
Therefore theoretically a change to lung structure caused by PE would cause a greater drop in arterial PO2 on exercise.
BUT...there is currently no evidence for using this in our diagnostic workup for PE (2)
How do we diagnose PE?
Canterbury Hospital Health Pathways recommends:
ALL patients with suspected PE should have:
- their pre-test probability assessed using the Revised Geneva scoring system
- AND have blood taken for a D-dimer assessment
Patients with signs of right ventricular dysfunction should have:
- urgent investigations with a CTPA and/or echo, as they may benefit from thrombolytic therapy using the standard tPA protocol
Out of normal working hours, and if it is clinically safe to delay establishing the diagnosis, consider anticoagulation overnight and investigate the following morning.
| Low Risk | Intermediate Risk | High Risk |
|---|---|---|
| < 4 points | 4-10 points | > 10 points |
The patient in the case had a Revised Geneva Score of 8 - intermediate risk - and a D dimer of 2050.
If the D-dimer is negative and:
- the patient has a low or intermediate pre-test probability, a clinically significant PE can be excluded
- the patient has a high pre-test probability, consider CTPA or VQ scans
If the D-dimer is positive with a normal CXR:
- VQ scanning or CTPA scanning should be considered.
Low/intermediate risk and:
- negative CTPA or normal VQ scan: excludes clinically significant PE.
- inconclusive VQ: investigate further with CTPA scanning.
- positive CTPA and/or high probability VQ: treat with anticoagulation.
High risk and:
- negative CTPA: may require further investigation with USS of leg veins or VQ scanning.
- positive CTPA and/or high or intermediate probability VQ: treat with anticoagulation.
The patient was admitted to medicine and had a CTPA which showed an isolated subsegmental PE (ISSPE) in his right upper lobe.
He was commenced on warfarin and treated for his cellulitis.
To treat, or not to treat, that is the other question…
There is much discussion as to whether patients with an isolated subsegmental PE (ISSPE) should be treated with anticoagulation as the risk/benefit in this cohort is unclear (3)
Studies appear to show that people with ISSPE have:
- a lower rate of mortality, morbidity and recurrence than those with larger PE
- comparable outcomes between those receiving anticoagulation and those who are not
- in some studies the outcomes of those not treated are the same as those who have not had a PE
However, there is not currently enough evidence to stop treating ISSPE patients.
Andy Neil, Emergency Medicine Ireland and Ryan Radecki, EM Literature of Note have also discussed this subgroup of PE patients.
Massive PE
In this group it is not a question of whether to treat or not, but how aggressively to treat.
This diagnosis should be considered in patients with severely compromised oxygenation or haemodynamics without other clear cause. (4)
It’s the THROMBUS part of the 4Hs and 4Ts of reversible causes of cardiac arrest.
Patients often present with severe dyspnoea, chest pain or syncope.
They can have non-specific examination features, tachypnoea, tachycardia and hypotension
+/- symptoms of right ventricular failure (increased JVP, parasternal heave, ECG showing S1Q3T3)
T wave inversion in precordial leads indicates severe RV dysfunction.
Management of Massive PE
- ABC
- Supplemental O2, intubation if indicated
- Fluid/pressor support
- CTPA
- Thrombolysis
- Clot retrieval
- Consider IVC filter
Suspected PE in Pregnancy
PE should be considered in all pregnant patients who present with chest pain and/or dyspnoea.
- Wells score and Revised Geneva score are not validated in pregnancy
- CTPA should be avoided in pregnant women if possible due radiation risk to the developing breast and foetus.
- A perfusion-only scan may be undertaken instead, depending on the gestation.
- A normal D-dimer level makes the diagnosis of PE very unlikely, but there is discussion around what the normal values should be during each trimester.
- A chest X-ray involves minimal radiation to both mother and fetus.
Canterbury Hospital Health Pathways for Suspected PE in Pregnancy:
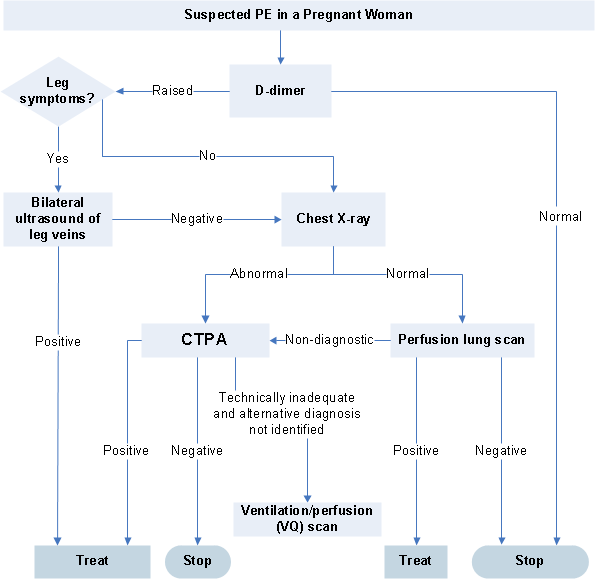
Summary
- Consider PE in patients with pleuritic chest pain and risk factors
- Risk stratify using a scoring system such as Revised Geneva
- Use the pre-test probability of PE in combination with the D-dimer to determine the need for imaging
- Eliciting chest wall tenderness and excluding desaturation after exercise can NOT be used to exclude PE
References
1) Chest wall tenderness: a useful discriminatory sign for PE? Hyun Choi 2003/2011, published in:
Best Bets
2) Exercise induced oxygen desaturation as a rule out tool for acute pulmonary embolism? Hyun Choi 2015, published in:
Best Bets
3) Do patients with a clinically suspected subsegmental pulmonary embolism need anticoagulation therapy? Chris Morgan, Hyun Choi 2015, published in:
Best Bets
4) Massive Pulmonary embolism. Victor F Tapson MD 2005 from:
UpToDate